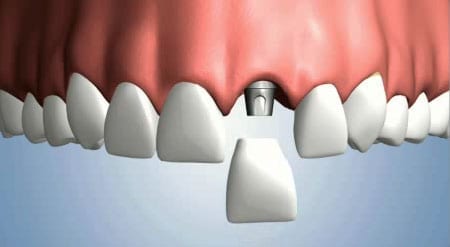
 Problems with dental implants are very rare when they are placed by an experienced oral surgeon, with implant success rates averaging around 97 percent and long-term implant survival rates also in the high 90 percent range, according to the Academy of Osseointegration. Of course, that means that roughly 3 of every 100 dental implants placed will fail, sometimes after they have been crowned. Other problems can occur after restoration is complete as well, which while still fairly uncommon, happen a bit more often than implant failure. However, many such complications are preventable with proper care, and most can be treated successfully.
Problems with dental implants are very rare when they are placed by an experienced oral surgeon, with implant success rates averaging around 97 percent and long-term implant survival rates also in the high 90 percent range, according to the Academy of Osseointegration. Of course, that means that roughly 3 of every 100 dental implants placed will fail, sometimes after they have been crowned. Other problems can occur after restoration is complete as well, which while still fairly uncommon, happen a bit more often than implant failure. However, many such complications are preventable with proper care, and most can be treated successfully.
Crown Movement
In a small percentage of patients, crown wobbling or movement can become an issue and should always prompt a visit to a dental professional as soon as possible. Wobbling or movement of the crown can happen for a number of reasons. Most common are improper seating of the crown on the implant abutment or loosening of the small screw that secures the abutment to the implant, issues that can be resolved with proper adjustment.
Rarely, the problem lies with the dental implants themselves losing their bond with the jawbone. Late implant failure, occurring after a successful osseointegration and restoration process, can most often be attributed to mechanical stress, with factors like an improper bite, teeth clenching or teeth grinding putting excessive pressure on the implant, causing it to loosen. Unfortunately, removal of the implant is usually necessary under such circumstances, although it can often, but not always, be replaced.
Peri-Implantitis
Peri-implantitis is an inflammatory condition that can affect the gum and bone tissue surrounding dental implants. It is quite similar to periodontal disease, commonly known as gum disease, with both caused by bacterial invasion.
Symptoms can include redness, swelling and irritation or pain in the gum tissues surrounding the implant, and often, there will be some bleeding of the gums during routine brushing and flossing. Peri-implantitis can cause gums to recede, exposing the implants, and if allowed to progress, can result in bone loss around dental implants, causing loosening and failure.
Bacteria can accumulate around the implant if the crown doesn’t fit quite right, leaving a tiny gap where it is fitted to the abutment, creating a space for bacteria that can lead to peri-implantitis to invade and multiply. Rough spots, such as those created by dental cement trapped under the gum, can provide a breeding ground for bacteria, as can insufficient cleaning, allowing dental plaque to accumulate.
Like gum disease, peri-implantitis can generally be cleared up with treatment. If a fault in the restoration is at the root of the infection, adjustments will be necessary to prevent recurrence of the disease.
Other possible problems that can occur after crowns have been loaded are wear or damage in the crowns, making repair or replacement necessary. Risk of complications with dental implant restoration is minimal when dental implant placement is carefully planned and skillfully performed by an by an experienced oral and maxillofacial surgeon.
